Evaluating the ocular surface prior to cataract or refractive surgery has become the norm. We know that ocular surface disease affects visual acuity, so cataract measurements of a patient with untreated dry eye may be inaccurate, resulting in subpar surgical outcomes along with exacerbated dry eye symptoms.
But I feel we need to go further: We should evaluate the ocular surface for all preoperative patients experiencing vision issues. Over the years, I have evaluated many patients for surgery, only to find their diagnosis is more complex and perhaps does not require surgery — including the man in this recent case.
PRESENTING COMPLAINT
A 22-year-old male patient was referred to me for a keratoconus evaluation and possible corneal collagen cross-linking. He had been complaining of blurred vision and photophobia, which had worsened over the previous few weeks. He was also complaining of ghost imaging in each eye and monocular diplopia. His optometrist identified possible early keratoconus and sent the patient to our office for a consultation.
EXAMINATION AND TESTING
When I examined the patient, his visual acuity (VA) was 20/40 OD and 20/50 OS. Fluorescein angiography showed he had grade 3 corneal staining OD and grade 2 OS. His tear osmolarity was 307 mOsms/L OD and 336 mOsms/L OS, and tear breakup time (TBUT) was 3 seconds OU.

The patient’s topography images showed irregular astigmatism and severe conical steepening in both eyes. They were significant cones, but they did not look like familiar keratoconus. That is, he appeared to have an atypical cone with superior steepening, rather than the inferior steepening typical of keratoconus.
DIAGNOSIS
The steepening seen in topography was not consistent with that of keratoconus. At the same time, the diminished VA, corneal staining, very low TBUT and high tear osmolarity OU (“high” defined as above 300 mOsms/L and an inter-eye difference greater than 8 mOsm/L) correlated strongly with severe dry eye disease, which was my diagnosis.
TREATMENT AND OUTCOMES
I felt that the patient’s dry eye might have been causing the irregular topography results. I ordered loteprednol etabonate ophthalmic gel (Lotemax, B+L) b.i.d. and preservative-free artificial tears p.r.n. The goal of the dry eye treatment was, first, to see if the topography was accurate, and second, to clean up the surface for the eventual treatment if warranted. If the tear film improved and the topography remained stable, I would be more convinced that the steepening was real.
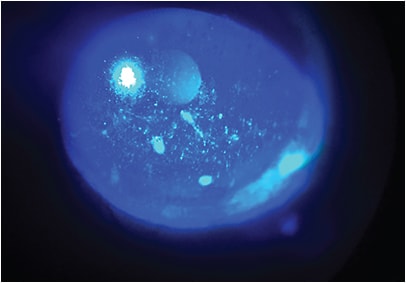
When the patient returned two weeks later, his VA had improved from 20/40 OD and 20/50 OS to 20/25 OU. His grade 2 and 3 corneal staining had resolved. What’s more, the patient’s steep topography had changed dramatically, flattening by 3 to 4 diopters and losing the cone-like appearance entirely, showing only mild astigmatism. His tear osmolarity decreased to 304 OD and 320 OS. The dry eye was clearly improving, but it was not completely resolved.
At this time, I instructed the patient to taper off the loteprednol and to begin lifitegrast (Xiidra, Shire) b.i.d. Because it appeared that his abnormal topography was related to ocular surface disease, rather than keratoconus, I did not schedule the patient for corneal cross-linking.
CONCLUSION
If I had not performed a thorough dry eye evaluation of this patient, I may have performed the corneal cross-linking despite his not having keratoconus. Surgeons should perform a detailed ocular surface evaluation prior to surgery, whether it is cataract surgery, refractive surgery, or even corneal cross-linking. Tear film osmolarity testing and TBUT are fast, reliable tools to help identify an abnormal tear film so that we do not overlook ocular surface conditions. For any patient who has poor vision, we need to determine the cause, and the tear film is an excellent place to start. OM









